Tramadol Seizure Risk Assessment Tool
Your Risk Profile
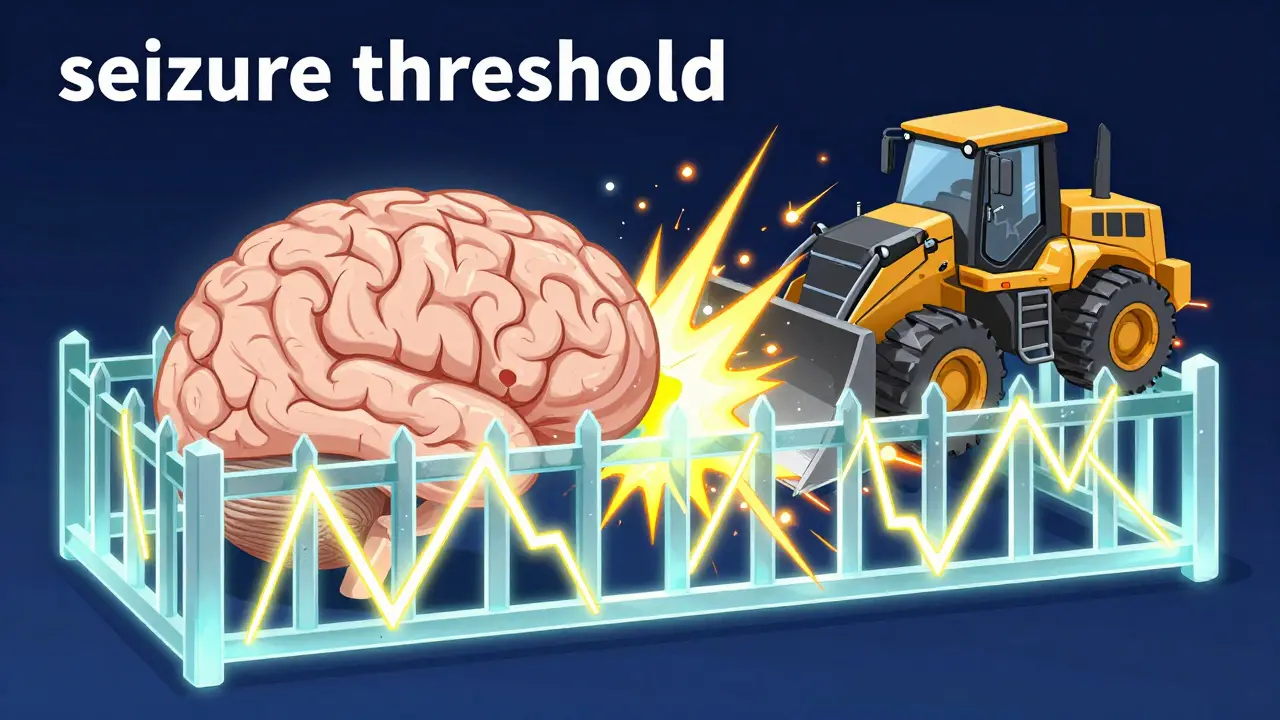
The core of the problem is what doctors call the "seizure threshold." Think of this as a mental fence. As long as your brain activity stays behind that fence, you don't have a seizure. Some drugs, including certain opioids, act like a bulldozer that knocks that fence down. When your threshold is lowered, it takes much less electrical stimulation to trigger a generalized tonic-clonic seizure. For someone who already has a seizure disorder, this isn't just a side effect; it's a major red flag.
How Tramadol Triggers Brain Activity
Most opioids just block pain signals. Tramadol is different because it plays a double game. It acts as a weak mu-opioid receptor agonist, but it also stops your brain from reabsorbing serotonin and norepinephrine. This dual-action mechanism is why it's effective for pain, but it's also why it's risky.
Research suggests that tramadol and its M1 metabolite might interfere with gamma-aminobutyric acid (GABA), which is the brain's primary inhibitory neurotransmitter. In simple terms, GABA acts like the brakes on your brain's electrical system. By inhibiting GABA, tramadol effectively cuts the brakes, making it much easier for the brain to slip into a seizure state. Interestingly, at very low doses, some animal studies suggest it might actually prevent seizures, but once you hit medium to high doses, it becomes pro-convulsant.
The Danger Zone: Dosing and Timing
You might think seizures only happen during an overdose, but that's a dangerous assumption. While the maximum recommended dose is 400mg per day, there are documented cases of patients having seizures at just 75mg per day. This proves that for some people, the biological risk is tied to their individual chemistry, not just the amount of pill they swallow.
Timing is also critical. Data from clinical studies show that the vast majority of tramadol-induced seizures happen within the first 24 hours of taking the drug. This window is the highest risk period. Interestingly, EEG tests often show abnormal brain activity during this initial window, but these abnormalities usually disappear within a week, meaning the neurological "storm" is often transient rather than a permanent brain injury.
| Feature | Traditional Opioids (e.g., Morphine) | Tramadol |
|---|---|---|
| Primary Mechanism | Mu-opioid receptor agonist | Dual: Opioid agonist + Serotonin/Norepinephrine reuptake inhibitor |
| Effect on Threshold | Generally neutral or anticonvulsant at low doses | Significantly lowers seizure threshold |
| Risk at Normal Dose | Very low | Present for susceptible individuals |
| Neurological Impact | Sedation/Respiratory depression | Potential for myoclonic activity and tonic-clonic seizures |
Dangerous Drug Combinations
Taking tramadol alone is risky for some, but adding other medications can turn a spark into a fire. This is where "polypharmacy"-taking multiple drugs at once-becomes a serious concern. If you are taking antidepressants or antipsychotics, the risk spikes.
Specifically, Tricyclic Antidepressants (TCAs) and Selective Serotonin Reuptake Inhibitors (SSRIs) can interact with tramadol's effect on serotonin. This doesn't just increase the risk of serotonin syndrome; it further destabilizes the seizure threshold. In real-world reports, patients who were stable on tramadol daily suddenly experienced seizures only after their dose was increased or after they added an antidepressant to their regimen.
Alcohol is another major culprit. Combining alcohol with tramadol significantly increases the likelihood of a seizure. The same goes for certain antipsychotic medications, which can further disrupt the electrical balance in the brain. If you are mixing these, you are essentially removing every safety barrier your brain has against a seizure.
Who is Most at Risk?
While anyone can theoretically react poorly, certain groups are in the line of fire. People with a pre-existing seizure disorder are the primary group; for them, tramadol is generally contraindicated, meaning it should not be used at all. Children under 12 are also strictly excluded from using this medication due to these risks.
Physical health also plays a role. People with renal impairment (kidney failure) are at a much higher risk. Because the kidneys are responsible for clearing the drug from your system, renal failure causes tramadol to build up in the bloodstream. This leads to higher concentrations of the drug in the brain, which can trigger a seizure even if the dose seems standard. There are recorded cases of patients with renal failure seizing after receiving intravenous doses that might be tolerated by someone with healthy kidneys.
Recognizing and Handling a Reaction
A tramadol-induced seizure usually presents as a generalized tonic-clonic seizure. This means the person loses consciousness, their muscles stiffen, and they experience rhythmic jerking. These are typically self-limiting, meaning they stop on their own, but they are still medical emergencies.
If you or a loved one is prescribed this medication, be vigilant during the first 24 hours. Watch for "aura" symptoms or myoclonic jerks (small, involuntary muscle twitches), which can be warning signs that the seizure threshold is dropping. If a seizure occurs, the immediate priority is safety-clearing the area of hard objects and ensuring the person is breathing-followed by emergency medical intervention.
Safer Alternatives and Next Steps
If you have a history of seizures, you don't have to go without pain relief. There are many other options that don't interfere with the brain's electrical stability. Non-opioid alternatives or different classes of analgesics can provide relief without the risk of triggering a neurological event.
The most important thing is to be honest with your doctor about your medical history. Tell them if you've ever had a faint, a blackout, or a diagnosed seizure disorder. Also, provide a full list of every supplement and medication you take, including over-the-counter antidepressants or sleep aids. A quick check of your medication list can be the difference between effective pain management and a trip to the emergency room.
Can I take Tramadol if I have epilepsy?
Generally, no. Clinical guidelines and medical authorities strongly contraindicate the use of tramadol in patients with seizure disorders because it significantly lowers the seizure threshold, making a breakthrough seizure much more likely.
Does the dose of Tramadol affect the seizure risk?
Yes, higher doses (especially those exceeding 400mg/day) increase the risk substantially. However, it is important to know that seizures have been reported even at normal therapeutic doses (such as 75mg/day) in susceptible individuals.
What medications make Tramadol more dangerous?
The risk is significantly higher when tramadol is combined with Tricyclic Antidepressants (TCAs), SSRIs, antipsychotics, or alcohol. These substances can interact with the brain's serotonin and norepinephrine levels, further lowering the seizure threshold.
When is the highest risk window for a seizure after taking Tramadol?
The highest risk occurs within the first 24 hours after taking the medication. Many documented cases of seizures happened during this initial window.
Does kidney disease affect how Tramadol works?
Yes. Since tramadol is cleared by the kidneys, people with renal impairment may experience a buildup of the drug in their system, which increases the risk of toxicity and seizures.



14 Comments