Imagine trying to bake a world-class gourmet cake, but you aren't given the recipe, the oven temperature, or even the exact brand of flour used. You only have a slice of the finished cake to study and a mandate to make an exact copy. That is essentially what developers face in biosimilar manufacturing is the process of creating biologic medical products that are highly similar to an already approved reference product. Unlike a simple chemical pill, these are massive, intricate molecules grown inside living cells. Because biological systems are naturally moody and variable, the stakes are incredibly high: a tiny tweak in the "kitchen" can result in a product that the human body rejects or one that simply doesn't work.
The "Process Defines the Product" Dilemma
In the world of traditional generics, chemistry is king. If you know the molecular structure of a drug, you can synthesize it in a lab with pinpoint precision. But with biosimilars, the rules change. The biologic medical products are so complex that the way they are made actually determines what the final product is. If you change the temperature of the incubator by a few degrees or shift the pH level of the nutrient broth, you change the protein itself.
This means developers have to reverse-engineer a "molecular fingerprint." They analyze the reference product and set strict limits on dozens of quality attributes. They aren't just copying a formula; they are trying to mimic an environment. If the original manufacturer used a specific cell line and a particular feeding schedule, the biosimilar developer has to find a way to get the same result without ever seeing the original proprietary blueprints.
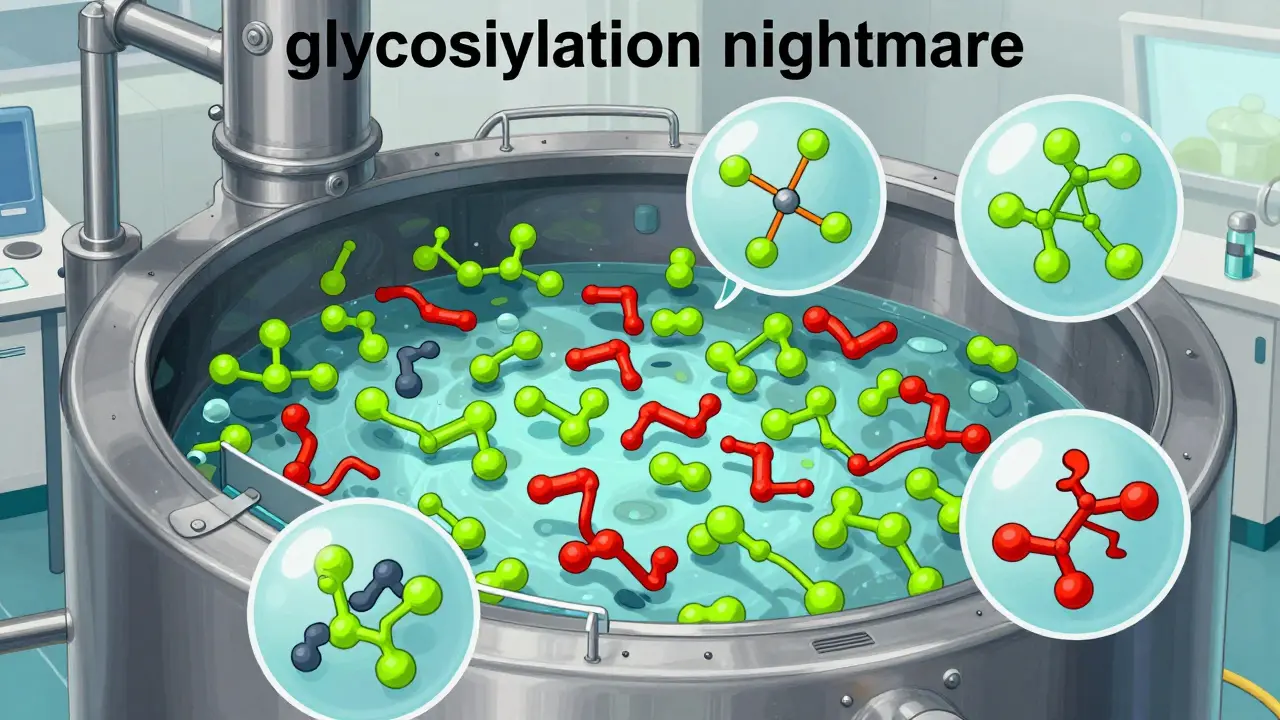
The Glycosylation Nightmare
One of the most frustrating hurdles in production is glycosylation patterns, which are the carbohydrate structures attached to protein backbones. Think of these as the "decorations" on the protein molecule. These sugars are incredibly sensitive. Factors like oxygen levels in the tank or the specific composition of the culture media can change how these sugars attach.
Why does this matter? Because if the glycosylation is off, the drug might be cleared from the patient's body too quickly, or worse, it could trigger an immune response. Achieving a match with the reference product requires a level of control that borders on the obsessive. You aren't just managing a chemical reaction; you're managing a living population of cells that can react unpredictably to the slightest environmental shift.
The Struggle of Scaling Up
Something that works in a small 5-liter lab beaker rarely works the same way in a 2,000-liter bioreactor. This is the classic "scale-up" problem. In a massive tank, mixing efficiency drops, and oxygen doesn't reach every cell equally. Temperature uniformity becomes a battle. If the cells at the bottom of the tank "feel" different than the cells at the top, the proteins they produce will vary.
Manufacturers have to carefully calibrate stirring speeds and aeration rates to ensure the cells remain happy and consistent. There's also the physical reality of equipment. Not every plant has the space or the budget to build the massive halls required for industrial-scale bioreactors. For mid-sized companies, the leap from pilot phase to commercial production is often the point where many projects fail due to the sheer cost of infrastructure.
| Feature | Small-Molecule Generics | Biosimilars |
|---|---|---|
| Structure | Simple, well-defined | Large, complex proteins |
| Production | Chemical synthesis | Living cell cultures |
| Consistency | Easily replicated | High batch-to-batch variability |
| Development Cost | Relatively low | Extremely high |
| Regulatory Path | Standardized (Bioequivalence) | Complex (Comparability exercise) |
Cold Chain Risks and Batch Consistency
Even after the protein is successfully grown, the danger isn't over. Biosimilars are fragile. They require strict cold chain management, meaning they must be kept at precise temperatures from the moment they leave the bioreactor until they reach the patient. A single failure in a refrigerator or a rough ride in a delivery truck can cause the proteins to unfold or clump, rendering the entire batch useless.
Then there is the issue of batch-to-batch consistency. In chemical synthesis, if you follow the steps, you get the same result every time. In biologics, nature introduces variability. Ensuring that Batch 100 is identical to Batch 1 requires an incredibly tight grip on the entire production lifecycle. This is especially true for newer, more complex versions like bispecific antibodies, which require extra purification and refolding steps, adding more points where the process can break down.
Navigating the Regulatory Maze
The technical struggle is matched by a regulatory one. Agencies like the FDA don't just take your word for it; they require a mountain of evidence. Manufacturers must use advanced analytical techniques to prove the biosimilar's critical quality attributes match the original. This requires state-of-the-art labs and a team of experts who can interpret complex data.
The guidelines are also constantly evolving. A process that was acceptable two years ago might need updating today to meet new standards. This adds a layer of financial risk, as developers must invest heavily in a process that might be subject to a regulatory shift mid-way through the approval pipeline.

Modern Solutions: Automation and Single-Use Tech
To stop the bleeding of costs and product loss, the industry is moving toward single-use technologies. Instead of massive stainless steel tanks that require hours of cleaning and validation, companies are using disposable plastic liners. This eliminates the risk of cross-contamination and allows a facility to switch between different products much faster.
Automation is also taking over. By using closed automated systems, manufacturers reduce human error-which is often the cause of contamination. Real-time monitoring tools now allow engineers to see exactly what is happening inside the bioreactor and make adjustments on the fly, rather than waiting until the end of a batch to realize something went wrong.
The Bottom Line for the Industry
The market is booming-projected to hit over $58 billion by 2030-but the barrier to entry is a fortress. Only those who can balance the science of living cells with the rigid requirements of global regulators will survive. As we move toward 2026 and beyond, the winners will be the ones who embrace continuous manufacturing and AI to predict quality issues before they happen. For everyone else, the complexity of biosimilar production remains a daunting obstacle.
Why are biosimilars not called generics?
Generics are exact chemical copies of small-molecule drugs. Biosimilars are made from living cells and are far too complex to be exact copies. They are "highly similar" but not identical to the original biologic, which is why they require a different, more rigorous approval process to prove they work the same way.
What is the biggest risk during biosimilar scale-up?
The biggest risk is the loss of product quality due to physical changes in the environment. As you move from a small lab scale to a massive bioreactor, factors like oxygen transfer, mixing efficiency, and temperature gradients change, which can alter the protein structure and glycosylation patterns.
How does single-use technology help manufacturers?
Single-use bioreactors and containers reduce the need for time-consuming cleaning and sterilization validation. This lowers the risk of contamination, allows for faster changeovers between different drug products, and reduces the initial capital investment needed for stainless steel infrastructure.
What happens if glycosylation patterns are incorrect?
Incorrect glycosylation can change how the drug interacts with the body. It may lead to faster clearance of the drug from the system (making it less effective) or cause the patient's immune system to recognize the drug as a foreign invader, potentially leading to dangerous allergic reactions.
Do all biosimilars require a cold chain?
Almost all do. Because they are proteins, they are thermally unstable. Exposure to temperatures outside a very narrow range can cause the molecules to denature or aggregate, which ruins the drug's potency and can make it unsafe for use.





11 Comments