That burning sensation rising up your chest is one of the most common-and exhausting-parts of pregnancy. You aren't alone; between 30% and 80% of pregnant people deal with heartburn, especially as the baby grows and hormones shift. The good news? There are effective ways to manage it without risking your baby's health. But navigating over-the-counter options can feel like a minefield. Which pill is safe? When should you take it? And what about those strong prescription drugs if the simple ones don't work?
This guide breaks down the three main categories of heartburn medications: antacids, H2 blockers, and proton pump inhibitors (PPIs). We’ll look at how they work, their safety profiles based on current medical consensus, and exactly when to reach for each one. Remember, while this information reflects current guidelines from major health organizations, always check with your healthcare provider before starting any new medication.
Why Heartburn Hits Harder During Pregnancy
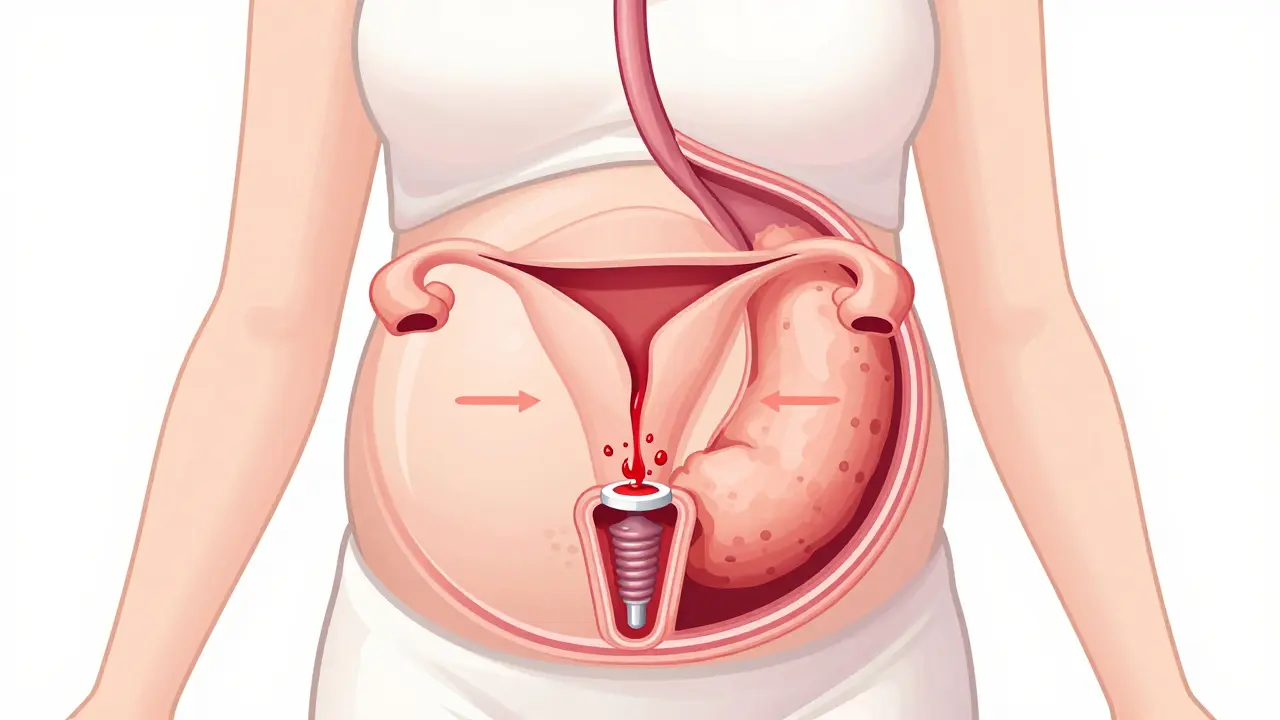
Before we talk pills, it helps to understand why this happens. It’s not just that your uterus is getting bigger. Two main factors drive pregnancy heartburn:
- Hormonal changes: Relaxin, a hormone that helps your body prepare for birth by loosening ligaments, also relaxes the valve between your stomach and esophagus. This lets acid creep upward.
- Physical pressure: As your baby grows, particularly in the second and third trimesters, your uterus pushes against your stomach, forcing acid up into your esophagus.
Symptoms often start early but tend to intensify later in pregnancy. While annoying, occasional heartburn is usually harmless. However, severe or persistent symptoms need attention because untreated GERD can lead to complications like esophagitis.
First Line of Defense: Antacids
When heartburn starts, doctors almost always recommend starting here. Antacids are considered the safest initial option because they work locally in the stomach and aren’t significantly absorbed into your bloodstream.
Why calcium carbonate? It neutralizes stomach acid quickly and provides a bonus: extra calcium for both you and your developing baby. According to Alliance OB/GYN, it is "probably the safest antacid" because calcium is essential for fetal bone development and maternal health.
Other common antacids include:
- Rolaids: Contains calcium carbonate and magnesium hydroxide.
- Mylanta: Often contains aluminum hydroxide, magnesium hydroxide, and simethicone (for gas).
Important warnings: Avoid antacids containing sodium bicarbonate (like Alka-Seltzer) as they can cause fluid retention and high blood pressure. Also, steer clear of bismuth subsalicylate (Pepto-Bismol) because it contains aspirin-like compounds that may harm the fetus. Some sources also advise limiting aluminum-containing antacids due to potential constipation or absorption issues.
How to use them: Take them after meals or when symptoms occur. Typical dosing is 500-1,500 mg of calcium carbonate every 4-6 hours as needed. Don’t exceed the recommended dose, as too much calcium can affect iron absorption.
Step Up Treatment: H2 Blockers
If antacids aren’t cutting it, your next step is likely an H2 blocker. These medications reduce the amount of acid your stomach produces rather than just neutralizing existing acid. They take longer to kick in (1-3 hours) but last longer (10-12 hours).
Famotidine has been extensively studied and is generally considered safe for short-term use under medical supervision. Another H2 blocker, cimetidine (Tagamet), is also sometimes used, but famotidine is often preferred due to fewer drug interactions.
A note on Ranitidine (Zantac): You might see older articles mentioning ranitidine. However, the FDA withdrew ranitidine from the U.S. market in April 2020 due to contamination with NDMA, a probable carcinogen. Do not use ranitidine during pregnancy.
Side effects: Headache or dizziness occurs in about 3-5% of users. If you experience these, talk to your doctor.
For Persistent Cases: Proton Pump Inhibitors (PPIs)
PPIs are the strongest acid reducers. They block the enzyme system in your stomach cells that creates acid. They’re reserved for cases where antacids and H2 blockers fail to provide relief.
Other PPIs like lansoprazole (Prevacid) and pantoprazole (Protonix) are also used, but omeprazole has the largest safety database. Medical News Today notes that while there may be theoretical risks, doctors prescribe PPIs when "the benefits outweigh the potential risks."
Safety concerns: A 2019 study in *JAMA Pediatrics* found a potential association between first-trimester PPI use and childhood asthma, though causation was not established. Because of this, most experts advise avoiding PPIs in the first trimester unless absolutely necessary. In the second and third trimesters, they are generally considered acceptable under strict medical supervision.
Onset and duration: PPIs take 1-4 hours to start working and can last 24+ hours. They are most effective when taken 30-60 minutes before a meal.
Timing Matters: Trimester-Specific Guidelines
Not all medications are created equal across all stages of pregnancy. Here’s a general breakdown:
| Trimester | Preferred Medication | Notes |
|---|---|---|
| First (Weeks 1-14) | Calcium Carbonate (Tums) | Avoid PPIs if possible. Minimize OTC meds. Focus on lifestyle changes. |
| Second (Weeks 15-27) | Antacids → Famotidine | More flexibility. H2 blockers are widely accepted. |
| Third (Weeks 28-40) | Antacids → H2 Blockers → PPIs | PPIs may be prescribed for severe GERD. Monitor calcium levels. |
Northeast Georgia Physicians Group advises avoiding most OTC medications in the first 14 weeks whenever possible. This is because organ formation is complete, and the risk of developmental harm is highest early on.
Lifestyle Changes That Actually Work
Medication isn’t the only tool. In fact, many women find significant relief through simple adjustments. Cleveland Clinic emphasizes these non-pharmacological strategies:
- Eat smaller, frequent meals: Large meals put more pressure on your stomach. Try five small meals instead of three large ones.
- Avoid trigger foods: Spicy, fried, acidic (citrus, tomato), and chocolate foods often worsen reflux.
- Wait before lying down: Stay upright for at least 3 hours after eating. Gravity helps keep acid down.
- Sleep elevated: Raise the head of your bed by 6-8 inches using blocks or a wedge pillow. Extra pillows alone often don’t work well.
- Wear loose clothing: Tight waistbands compress your stomach.
When to Call Your Doctor
While heartburn is common, some symptoms signal something more serious. Contact your provider immediately if you experience:
- Persistent pain that doesn’t improve with antacids
- Difficulty swallowing
- Unexplained weight loss
- Vomiting blood or material that looks like coffee grounds
- Black, tarry stools
These could indicate esophagitis, ulcers, or other conditions requiring specific treatment.
Is it safe to take Tums every day during pregnancy?
Yes, calcium carbonate (Tums) is generally safe for daily use as directed. It provides both heartburn relief and supplemental calcium. However, do not exceed the recommended dose (usually 500-1500 mg per dose, 4-6 times daily) as excessive calcium can interfere with iron absorption and cause constipation.
Can I take Pepcid (famotidine) in my first trimester?
Famotidine is generally considered safe, but many doctors prefer to avoid all non-essential medications in the first trimester (first 14 weeks) due to critical organ development. Start with antacids and lifestyle changes first. If symptoms are severe, consult your OB/GYN before taking famotidine.
Are proton pump inhibitors (PPIs) safe for breastfeeding?
Most PPIs, including omeprazole, are considered compatible with breastfeeding. Small amounts pass into breast milk, but studies show no adverse effects on infants. Always discuss with your pediatrician and OB/GYN to choose the lowest effective dose.
What should I avoid taking for heartburn while pregnant?
Avoid Pepto-Bismol (contains aspirin/salicylates), ranitidine (Zantac, withdrawn due to contamination), and antacids with high sodium content (can raise blood pressure). Also avoid combination products that include decongestants or pain relievers unless approved by your doctor.
Does heartburn mean my baby’s hair is growing?
This is a common myth! The old wives’ tale suggests severe heartburn means the baby will have thick hair. There is no scientific evidence linking heartburn severity to fetal hair growth. Heartburn is caused by hormonal relaxation of the esophageal valve and physical pressure from the uterus.